One Kentucky woman's heart-wrenching decision to end her health care nightmare
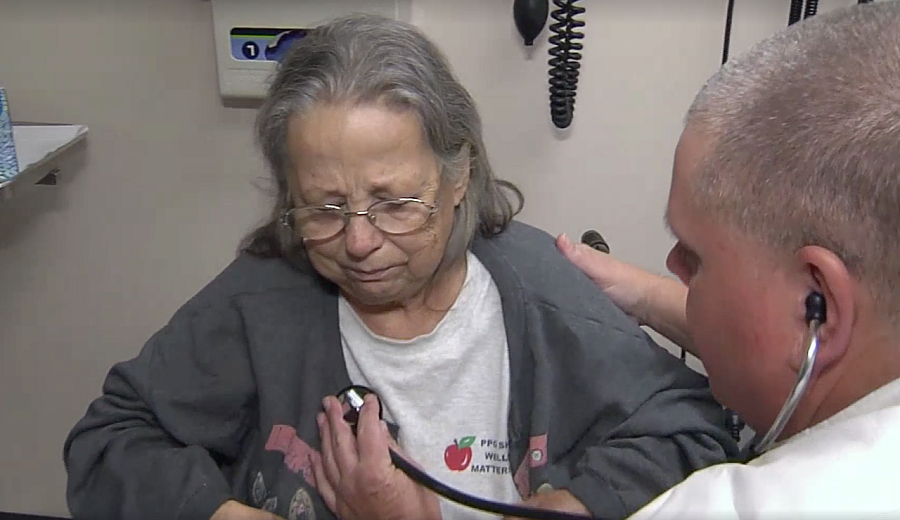
Susan Moore, suffering from colon cancer, could not afford basic care and was on the verge of giving up. (Image via Tracie Potts/NBC)
When I traveled to rural Kentucky seeking stories about the impact of health reform, I expected to see poverty. I didn't expect to end up sitting in an exam room in tears, trying to convince an elderly woman not to make a decision that would end her life.
“I'm dying and that's OK with me,” she told me. “It's just getting harder and harder, and I'd rather just quit.”
Susan Moore has colon cancer. She couldn’t afford transportation to dialysis three times a week. Medicare and Medicaid stopped paying. Medical staff at her Whitesburg, Kentucky clinic told me the local medical transportation service laid off workers because the county was experiencing its own financial challenges. This is the heart of Appalachia. Jobs are in short supply. So is money.
So is Susan's patience. And hope.
She made a conscious choice to stop dialysis, fully aware that she would not survive. The stress of bills she couldn't afford piling up and no way to get to treatments caused Susan to give up on life. And she was quite determined about it.
“I signed a DNR for the ambulance guys and the doctor so they know what my wishes are," she told me. “I’m not giving my kids the power to make my decisions when I already know what I want.”
Susan told me could barely afford food — she sets aside $70 at the beginning of the month to buy food for herself and her son. Her husband’s social security just wasn't enough to cover necessities and medical bills. She’s not alone. The median income in Letcher County, Kentucky is $21,110. Per capita income is almost half that, $11,984. Nearly a quarter of the county's families fall below the poverty line. Eight in 10 voted for President Trump. Now many are begging him not to gut the Affordable Care Act.
To find out why, I sat down for a frank discussion with Mike Caudill, CEO of Mountain Comprehensive Health Corporation. He runs a network of 20 stand-alone and school-based community health centers in southeastern Kentucky serving 30,000 patients a year. The clinic we visited is a 75,000-square-foot state-of-the-art building with dental, optometry, therapy and rehabilitation, and a full-service laboratory on site. It's fantastic health care with extensive access — but can patients afford it? Caudill says the combination of ACA and Medicaid cuts and loss of community health funding (also in limbo in Washington) will force him to close 14 clinics, including 6 in schools, and lay off 100 employees. That's just over a quarter of his staff. The health group also runs the county's only daycare, which could be in jeopardy without those funds.
My heart aches for his patients — especially Susan. Every story we heard was powerful, but none touched my heart like hers.
One of the hardest things about reporting is leaving people behind: telling their stories, but not sticking around to see how those stories end. For Susan, we have some idea. A viewer saw her story on social media and started a GoFundMe page that netted more than $17,000 in donations in just days. She's working with a local attorney to set up a trust so the distributions can benefit Susan but not affect her Medicaid eligibility.
I spoke with Susan recently. She's more upbeat but nervous about upcoming cataract surgery on both eyes. I tried to reassure her, having recently helped a relative after that same surgery. The donations should cover her out-of-pocket costs.
Things are working out. But how many more Susans are out there waiting on Washington to act?
