Access Denied: Oklahoma's Health-Care Crisis
Is Oklahoma headed toward a crisis in access to health care? Health experts say yes -- for many reasons. This three-part series takes a look at the problems, how it affects all Oklahomans and what can be done to change it.
Part 1: Physician shortage contributes to looming health-care crisis
Part 2: Rural Oklahoma health-care needs underserved, area lacks specialists
Part 3: Mid-level practitioners vital to sustain post-reform health care
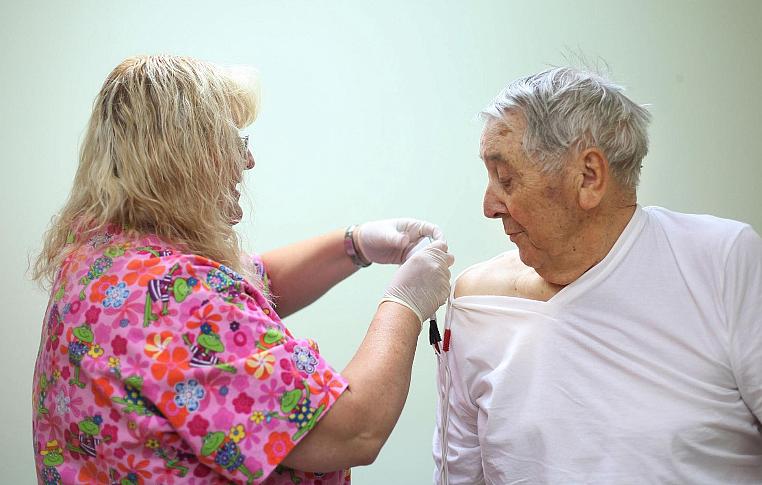
Ray Ingram, 86, gets help with shock therapy from clinic employee Kelly Dority at Helton Rural Health Clinic in Coalgate, Okla. on June 17, 2011. Ingram, who lives around the corner from the clinic, came to the clinic with shoulder problems. Ingram has been seeing Dr. Richard Helton for 30 years.
Editor's note: Shannon Muchmore wrote this story as part of the California Endowment Health Journalism Fellowships, a program of the University of Southern California's Annenberg School for Communication & Journalism.
There are no cardiologists in virtually the entire northwest quadrant of Oklahoma.
The north Tulsa ZIP codes with the lowest life expectancy are also the ZIP codes with the fewest doctors.
Coal County has only one physician to care for its population of 6,000.
These and many other significant geographic disparities in the number of doctors per capita exist within Tulsa and the state.
Specialists, including cardiologists and oncologists, are clustered in metropolitan areas of Oklahoma but are scarce or nonexistent in rural areas of the state, according to a Tulsa World analysis. The World reviewed data from the Oklahoma Medical Board of Licensure and Supervision and the Oklahoma State Board of Osteopathic Examiners.
This barrier to access for people in less populated areas of the state often causes a delay in treatment or lack of preventive health services, health experts said.
Only 12 counties have an oncologist, a doctor who treats cancer patients. They are heavily concentrated in central and northeastern parts of the state.
Oklahoma has 36 counties with fewer than five family practice doctors, and at least four counties have none. Once again, the northwest and southeast sections of the state are poorly represented.
Life of the rural doctor
"You're out here on your own, and you have to make do," said Dr. Richard Helton of Coalgate, the lone physician in Coal County, in southeastern Oklahoma.
Helton works at the Helton Rural Health Clinic and also sees patients at Mary Hurley Hospital, which has 20 beds, and the 75-bed nursing home next door.
He sees all ages for all kinds of reasons and is on-call every weekday. Some patients call him R.J. and are eager to talk and see how he is. He ends most patient visits with, "God bless you."
Bethel Lee, 99, has lived in the nursing home for about two years.
"I forget these doctors' names except for Dr. Helton," she said. "I'll never forget his."
Ray Ingram, 86, has lived in Coalgate for 35 years. He visited Helton recently for a heart checkup. He doesn't know what the town would do without Helton's clinic.
"That's going to be a problem, really," he said.
Helton was born in Texas and grew up in Oklahoma. He went to medical school at Oklahoma State University and began practicing in Coalgate in 1981. He has a wife and two grown children and likes the rural life, he said.
In his 50s, Helton has no plans to retire any time soon and said he will always ensure his patients are cared for. Those who need specialists drive to Tulsa or Oklahoma City. Sometimes they are taken by ambulance.
"I try to do what I can to get my patients access to medical care," he said.
Geographic disparities
Coal County has about 51 health-care providers, including physician assistants and advanced practice nurses, per 100,000 people. The only county with a lower provider rate is Washita, which has about 34 providers per 100,000 people, according to the Oklahoma State Department of Health. There are 213 providers per 100,000 people statewide, according to a Tulsa World analysis.
About half of Oklahomans live in a rural area, and 68 of the state's 77 counties are classified as rural. Residents in those areas tend to be older, poorer and less educated than those in urban areas and they have less access to health care, according to the OSU Center for Rural Health.
This is particularly true for primary care, as Oklahoma was ranked 44th in the nation in access to a primary care physician in a 2011 report by the American Medical Association.
"We see some people come in here with chronic illnesses that if it had been caught earlier they would have had a better quality of life, for sure," said Lee Simpson, a physician assistant at the Helton Clinic in Coalgate.
Within Tulsa there are also geographic disparities. Northern and western areas have few physicians and even fewer specialists. The ZIP codes with the lowest life expectancy in the Tulsa area - 74126, 74106, 74116 and 74127 - are also the ZIP codes with the fewest doctors.
Those areas also have the highest minority population.
These disparities are the impetus behind the decision to locate the University of Oklahoma-Tulsa's Wayman Tisdale Specialty Clinic at 36th Street North and Hartford Avenue.
At a ceremony earlier this year to note a landmark in construction of the building, expected to open in the spring, City Councilor Jack Henderson was jubilant about the new facility. Henderson's district includes some of those ZIP codes with the lowest life expectancies.
"I cannot wait until we open these doors to the citizens who need these services so badly," he said then.
The doctor is in ... another town
Nationally, more than half of patients whom rural physicians refer to specialists have to travel 20 miles or more, according to a report by United Health Group, a large health-care company.
The report, released earlier this year, found that people in rural areas have a greater prevalence of chronic conditions such as diabetes, hypertension, cancer, arthritis and bronchitis. They are also more likely to report only "fair" or "poor" health.
As many as half of Americans live in a rural area, according to the U.S. Census Bureau.
Eleven percent of primary care providers are in rural areas, meaning there are 65 of them per 100,000 residents of the United States. The ratio is 39 per 100,000 in remote rural areas of the south, according to the report.
James Hess, chief operating officer with the OSU Center for Health Sciences, said it can be difficult to get physicians to locate in a rural area, where the lifestyle is different and Medicaid/Medicare reimbursement rates are lower.
The average medical school debt is more than $150,000, according to the American Medical Association.
Hess said there should be incentives such as loan forgiveness or repayment for physicians who establish a practice in rural, underserved areas. Also, junior high and high schools in rural areas need to promote science, math and other subjects that can lead to the medical profession, he said.
About 80 percent of medical students who go to college and do their residency in Oklahoma will end up locating in the state, Hess said.
"The only way to get people to go to rural Oklahoma is to recruit them from rural Oklahoma," he said.
