Virtual medical care leads to suffering for patients on the wrong side of the digital divide
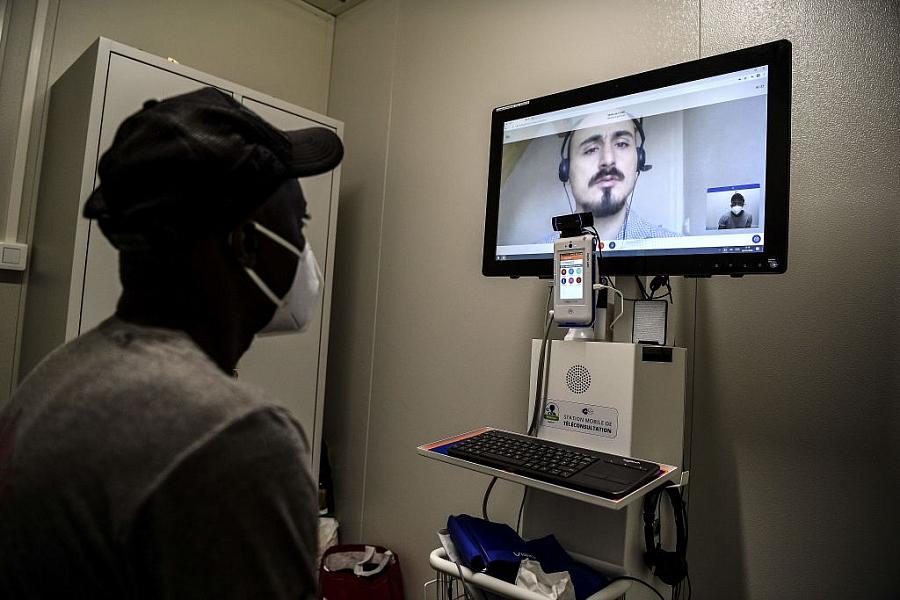
(Photo by Christophe Archambault/AFP via Getty Images)
As a family medicine physician, I have provided virtual care in the past but never to the degree I do now that COVID-19 has moved so much medical practice to phone and video. While this shift allows many patients to receive safe, timely care, the digital divide is causing blatantly disproportionate suffering by patients of color and those with limited English proficiency. And no institution or organization has yet taken responsibility to close the gap. The problem became all too real for me in a recent interaction with a 35-year-old Somali-speaking patient.
On our first call, the man’s interpreter told me he had started a new medication for his acid reflux, omeprazole, but felt the drug was making him feel ill. When I attempted to clarify, the interpreter simply repeated the phrase “feeling ill.” I wanted more information, but the patient did not have the technology to participate in a video visit, or a cuff to check his own blood pressure. After a lengthy discussion, we agreed to change his medication and follow up if the symptoms did not improve.
And they didn’t. In a phone visit a few weeks later, he said he felt dizzy. I told him he might be dehydrated, and drinking more fluids may help. As I considered the next step, the interpreter stated with equanimity, “He says he doesn't feel well. Something is going on. He feels like he's dying.”
My concern escalated. If the patient had been in my office, I could have relied on his gestures and facial expressions to understand his distress. If we had been able to talk directly, rather than through an interpreter, I could have heard his distress in his vocal tone, speed, and variation. Instead, I had to rely on the interpreter's plain, detached words, and I almost missed the urgency of the situation. I advised him to go to the ER. There he was found to have a hemoglobin level of 1.9. Normal level of hemoglobin — the protein responsible for carrying oxygen — is greater than 13.5. He was on the brink of death, and I had almost missed it.
Phone calls with interpreters are stripped of many details that help communicate a patient's illness. We often make decisions with incomplete and imperfect information in medicine, and relying on phone visits exacerbates the uncertainty. With better access to technology, many patients would receive better care. They could take photos of their rashes with their smartphone to send to me through the patient portal of the integrated health care system where I work. They could measure and record their blood pressure at home and share the results through our instant messaging system or in a video visit.
Unfortunately, many of my immigrant and Black patients do not have the technology or the digital literacy to use the tools available to communicate essential information about their conditions. For these patients, I have only two options: 1) manage their disease over a phone call with incomplete information, or 2) bring them to my office and expose them repeatedly, and unnecessarily, to the risk of acquiring COVID-19. For the Somali patient I cared for, I struggled to choose between an inadequate and an unsafe option.
My concern escalated. If the patient had been in my office, I could have relied on his gestures and facial expressions to understand his distress. If we had been able to talk directly, rather than through an interpreter, I could have heard his distress in his vocal tone, speed, and variation.
After countless failures of the system to provide adequate care, similar to what had happened with my Somali patient, I, along with several other physicians, advocated for our health care system to address the problem. We urged our system leaders to identify patients who do not have web-enabled devices or the knowledge to navigate our complicated website in English, and provide them with subsidized devices and training.
Our repeated calls for action were met with quick and curt replies.
Leaders of our health care system said the problem was “outside the scope” of current virtual care improvement initiatives. They said we needed to focus our efforts on what we knew and what we could control rather than invest in resource-intense social and technological interventions to bridge the digital divide — especially when there was no clear return on investment. We could give our patients a phone number to call to sign up for the online patient
portal, but it was not our role to make sure they had the technology and the ability to use that portal.
After all the conversations, I saw my system surrender to the reality of two-tiered care. The system would continue to create solutions and improvement initiatives assuming patients could access our virtual care options. For patients who could not, we would have a second set of processes that relied on phone calls and office visits. Let someone else bridge the digital divide.
I wanted my health care system to step up to solve the problem, because when we ignore issues of access that substantially alter the type and the quality of care, I am the one forced to provide unsafe and inequitable treatment. However, my system is not unique in its reluctance to address problems outside of health care.
We often want the health sector, with its sheer size and resources, to address social and political problems that are root causes of illness. We argue that social issues such as housing insecurity need to be addressed by the health care system because they exacerbate suffering and illness of patients and lead to worse health outcomes. But despite having the power and resources to make the changes, the health care sector has not adequately addressed the social determinants of health.
Prominent experts in the field — such as Don Berwick, former head of CMS and president emeritus of the Institute for Healthcare Improvement, and Alan Weil, editor-in-chief of Health Affairs — declare that health care organizations choose not to address these issues because they are designed to maximize financial returns and pursue growth. This design makes it implausible that they will ever “authentically and equitably engage with resource-poor communities” to solve large-scale social problems.
If the health-care sector does not have the will or the incentive to address unequal access to technology, the next hope would be for the government to do it. But I have yet to see a coordinated effort by federal or local governments to close the digital divide by providing all constituents with access to the right technology and the education to use it. The federal government has not updated its plan to expand broadband access in nearly a decade. Given our current climate, when the government cannot even institute a universal masking policy, despite mounting evidence, to stop the pandemic, I have little hope that it will focus on broadband equity. State governments have made their own plans to expand broadband access but these do not sufficiently address the needs of the many people who don’t own a device that uses broadband.
With the rapid expansion of telehealth, smartphones, tablets, and laptops aren’t luxuries — they are requisite for high-quality medical care. I commit to listening more attentively during phone calls, but that is not enough. Until we find a way to get health care leaders or policymakers to take responsibility for closing the digital divide, patients of color, poor patients, and those with limited English will suffer unnecessarily.
Raj Sundar, M.D., is a family medicine physician in Seattle. His work has been published in multiple journals including Health Affairs and Annals of Family Medicine.

