Access Denied: Oklahoma's Health Care Crisis
Is Oklahoma headed toward a crisis in access to health care? Health experts say yes -- for many reasons. This three-part series takes a look at the problems, how it affects all Oklahomans and what can be done to change it.
Today: Why Oklahoma faces a crisis in access to health care.
Sunday: A look at disparities across the state in access to health care.
Monday: Mid-level practitioners are among the solutions to providing care.

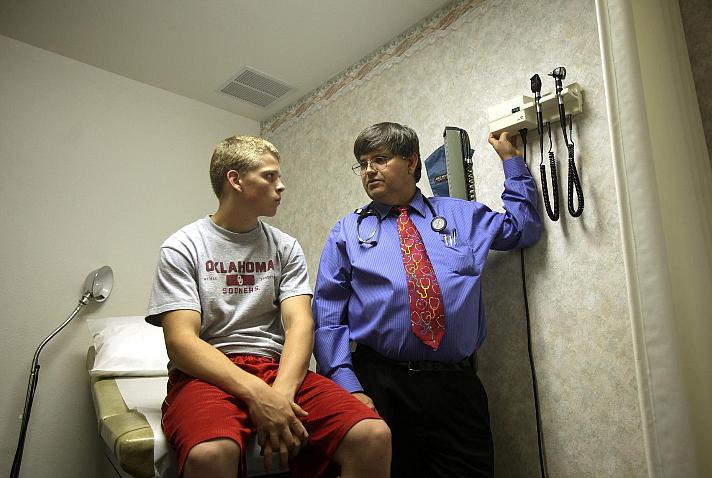
Dr. Michael Woods of Ramona treats Randy Ramsey, 17, of Vera, for a small granuloma. Woods is one of few doctors in the state doing family practice care in a rural setting.
Editor's note: Shannon Muchmore wrote this story as part of the California Endowment Health Journalism Fellowships, a program of the University of Southern California's Annenberg School for Communication & Journalism.
Dr. Michael Woods may deliver a baby in the morning, sign a death certificate in the afternoon and go to the high school football game that night to watch for injuries.
Clad in cowboy boots and often a quirky tie, Woods is counted on to give medical care of all kinds in his small community.
"For me it was just the comfort of being in a rural area, and I wanted to raise a family in a rural environment," said Woods, who works in Ramona, south of Bartlesville.
Oklahoma needs a lot more doctors like him.
Multiple factors are converging to create a looming health-care crisis in Oklahoma.
Physicians are mostly concentrated in Oklahoma City and Tulsa, while western and southeastern parts of the state have few doctors and even fewer specialists, according to a Tulsa World analysis of state medical board data.
There are 2.13 physicians for every 100 people in the state, according to the analysis. That number ranges from a low of 0.17 in Coal County to a high of 4.11 in Oklahoma County.
Oklahoma has more than 200 Health Professional Shortage Areas, meaning they don't meet the national standard of one physician for every 3,500 people. Those areas exist in 66 of the state's 77 counties.
The Tulsa ZIP codes with the lowest life expectancy are also the ZIP codes with the fewest doctors. These are 74126, 74106, 74116 and 74127. South Tulsa, midtown and surrounding suburbs boast many medical practices, but north and west Tulsa have far fewer.
The state is facing a severe shortage of doctors as the population ages. Adding to that, as many as 180,000 people are poised to receive insurance when provisions of federal health-care reform kick in 2 1/2 years from now.
Rural areas and already underserved urban areas will be particularly hard hit, with little access to specialists or doctors in general and a lack of public transportation options.
A worsening problem
An article in the February 2011 issue of the New England Journal of Medicine ranked Oklahoma as the most access-challenged state in terms of health care. The high number of currently uninsured residents and the relatively low number of primary-care providers in the state will present a significant challenge for patients seeking care, health policy experts said.
People who already have insurance could see increased waiting times. This may send patients to the emergency room, creating crowded conditions and driving up the cost of care.
The country as a whole is facing a shortage of as many as 150,000 physicians. That ratio of patients to physicians could increase by 25 percent, assuming federal health-care reform measures proceed and more people get health coverage.
Meanwhile, by 2030, nearly 1 in 5 Americans will be 65 or older, and the 85-and-older population will more than triple by 2050, according to the U.S. Census Bureau.
In Oklahoma, 1 in 4 doctors is older than 60, and their average age is 54. Many will be retiring soon.
Several issues are contributing to Oklahoma's physician shortage.
Medical schools are not increasing their class sizes, residency slots are hard to come by, and doctors are choosing to locate in other states.
The last two factors go hand-in-hand, as doctors often practice where they have their residencies. Without a connection, they have little reason to locate in a rural area.
The state is not well-positioned to handle a further deterioration in its health-care system. Oklahoma consistently ranks among the worst states for obesity, diabetes, smoking, heart disease and overall health. It has the least improvement in the country in age-adjusted death rate since 1990.
Shifting priorities
Woods, 56, moved to Ramona in 1987 and opened up a tiny practice across from the high school. He is the essence of a primary-care physician, practicing everything from prenatal care to geriatrics.
He goes to all the home football games and rushes to the field if a player is injured. He is the medical director for five rural fire departments in the area and keeps up with the local school superintendent when flu season hits.
He grew up on a farm and never really wanted to live in the city. Woods wanted to raise his family in a rural area, so he settled in Ramona.
In the first few years of his practice, he saw a lot of patients he diagnosed with cancer. They hadn't gone to see a doctor earlier because there wasn't one nearby.
"If people don't have a way to easily get in to see a physician close to where they live, they won't come in," he said.
John Silva, CEO of Morton Comprehensive Health Services, a federally qualified health center in Tulsa, said some areas in Oklahoma have no provider at all.
He lamented the decision of Gov. Mary Fallin earlier this year to return $54 million in federal money meant to help the state set up a health insurance exchange, which is a website to help consumers comparison shop for insurance.
"I am absolutely astounded that in a state with the level of health disparities that exist that we have leadership that says things like, 'We don't need federal money; we can take care of our own,' " Silva said. "If that were true, then we wouldn't have infant mortality, obesity, diabetes, cardiovascular issues that are astounding in America in 2011. And yet we object to federal investment."
There has to be a statewide dialogue about priorities, he said, and political bickering and legislative special interests must be shelved in order to move forward.
Building new facilities should not necessarily be the method for improving health care, Silva said, and the use of emergency rooms as a place for primary care needs to change.
"We continue to do the same old things and then wonder why nothing seems to improve," he said.
Financial challenge
The lack of residency slots available for graduate medical students is one of the stickiest problems Oklahoma faces. Residency compensation is paid through federal dollars, but the amount has been frozen since 1996. New residency programs aren't available for reimbursement during the first three years, after which point the facility is not permitted to add any new residency positions for the duration of the program's existence.
Graduate medical education also remains on the federal chopping block for further cuts as budget negotiations continue in Washington.
Medical schools can try to increase class sizes to help make up for the physician shortage, but with the current situation, it wouldn't do much good, said Howard Barnett, president of the Oklahoma State University Center for Health Sciences.
"We really are determined to meet that need," he said. "But if we don't have the residency slots, it's a fool's errand."
James Hess, chief operating officer for the OSU Center for Health Sciences, said the pending crisis is predictable and understood.
"There isn't anything about this problem that money won't solve," he said.
One afternoon in his clinic, Woods oversaw care for a woman needing a referral, a woman with a pain in her right side and a teenager with a knot on his arm, probably from playing football.
Dr. Kimberly Young, a resident at the clinic, talked to the patients and dealt with their concerns. Then she talked to Woods about each patient, and they went through treatment decisions.
Randy Ramsey, 17, decided to get the knot on his arm removed after a consultation with Woods determined it was likely a granuloma, a benign inflammation in the skin. They performed the quick procedure in the office, and Ramsey and his father were on their way.
Young, 29, grew up in tiny Ellis, Kan., where the county hospital had 25 beds.
She likes the rural life and wasn't going to let the promise of more money lure her into a specialty when she prefers primary care in a small setting.
"I want to be that person that everyone knows in the town and respects but also trusts," she said.

